A Comprehensive Guide to a Comprehensive EHR System

In this guide, you can read about the electronic health records software market; the difference between EMR and EHR systems. We will discuss EHR software features and benefits, as well as the most critical stages of EHR system development.
***
The Healthcare industry is in rough shape. Even before the events of the past two years, US hospitals dealt with decreasing revenues. As well as “a mismatch between organizations’ strategies and actual market demand and a lack of operational discipline.”
Now, hospitals all over the world are dealing with overflowing facilities, lack of personnel and supplies. The pandemic also put a strain on the management. It is testing its crisis-management skills to their limits.
The industry requires every bit of help it can take. Investing and rising salaries can help deal with the lack of personnel and supplies. The software, in turn, can optimize and automate processes. Electronic health record systems in particular can reduce the amount of paperwork. Also, they decrease workload and improve patient management.
What is EHR in HealthCare?
EHR system (electronic health record) is a universal software system. It stores, manages, and transfers all patient data. These systems ensure all establishments involved in care have access to relevant information. On top of that, EHR can have extra features that make medical care more accessible to patients. They are telemedicine, voice recognition, billing features, etc.
In essence, EHR systems exist to emulate an ideal scenario — regardless of the circumstances, each patient is always treated by a medical professional who knows everything about the patient’s history and medical records.
Managing and transferring patient data have always been a source of insufficient care and frustration. As well as overhead costs, mistakes, and wasted time in the HealthCare industry. EHR systems address these issues and streamline patient management and care.
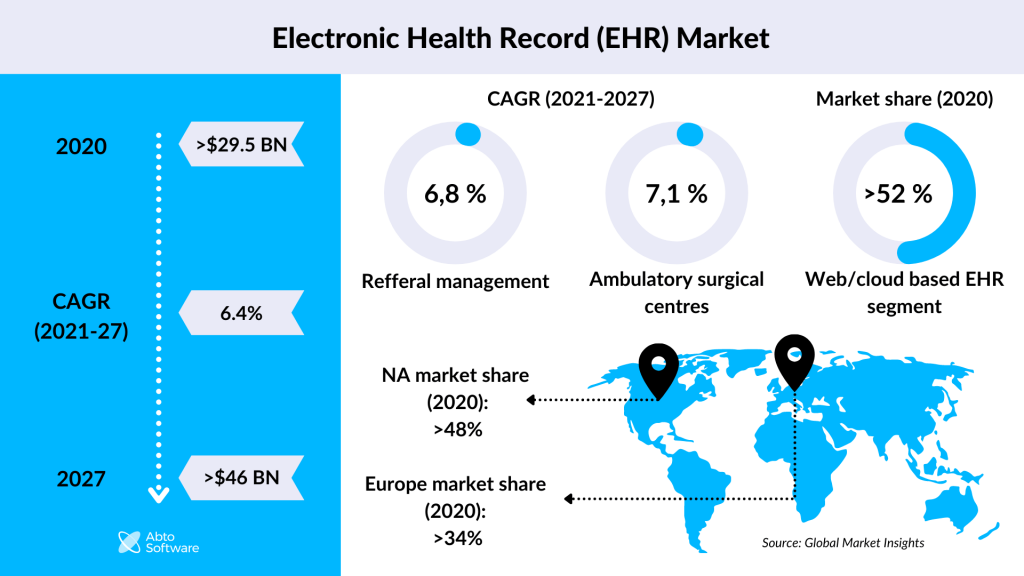
What is the difference between EHR and EMR?
During your online searches, you may have stumbled upon two separate programs: EHR (electronic health record) and EMR (electronic medical record) systems. Though on the surface level, both software systems seem very similar or even synonymous, that’s a deceptive similarity. (Some people use the terms interchangeably, but it means ignoring the difference between the two)
What is the difference between EHR and EMR?
EMR is “a digital version of the paper charts in the clinician’s office.” The system contains and helps manage and track patient data in a single medical practice. It also helps monitor the quality of medical care on the scale of a single practice/medical facility. In essence, EMR is a rigid, localized system that exists to serve a single establishment.
EHR, on the other hand, is an EMR on steroids. An EHR system contains everything EMR does. But it also can span the entirety of all parties that take part in a patient’s care, hospitals, laboratories, individual specialists. Such a system allows for quick and simple transfer of data between the parties. Also, it helps with close monitoring and management of all nuances of patient care.


EHR software features
What are the features of an EHR system? Well, electronic health record systems can have slightly different functionality based on the customer’s requirements and circumstances.
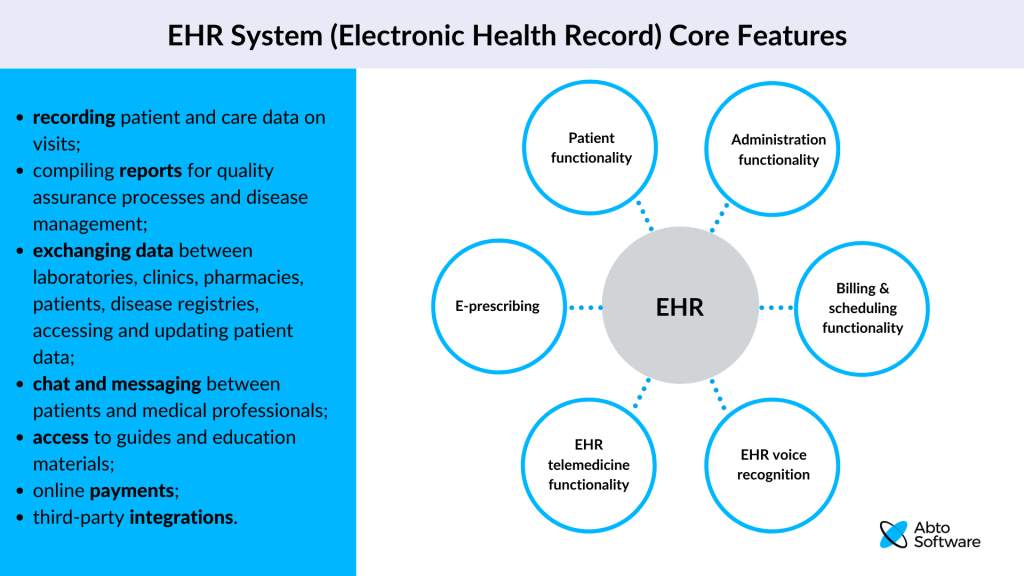
But, in general, any fully-developed EHR software should have the following features:
Core health records and administration functionality
Recording patient and care data on visits; compiling reports for financial management, quality assurance processes, and disease management; functionality for exchanging data between laboratories, clinics, pharmacies, patients, disease registries, etc.; commonly used forms and templates for various documentation in use by the facilities.
Billing & scheduling functionality
For scheduling and monitoring visits and billing patients.
Medication reconciliation
Comparing newly prescribed medication to the medication in use to avoid dangerous or unwanted overlaps.
E-prescribing or electronic prescribing
For sending custom prescriptions directly to pharmacies.
EHR telemedicine functionality
Using audio and video to connect patients and medical professionals across the globe.
EHR voice recognition
Using speech-to-text recognition to input data and navigate EHR.
Patient functionality
Accessing their patient data with the ability to update some general information if needed; scheduling appointments; chat and messaging with healthcare providers; access to relevant guides and education materials; conducting online payments; third-party integrations.
All the subsystems, modules, and different EHR software features should work seamlessly together and interact where it’s required.
Types of EHR systems
There isn’t a rigid division of EHR software into different types. Though, one can categorize those systems based on the data hosting approach.
In this case, there are two main types of EHR systems:
- Physician-hosted systems. All the data is stored and processed on the on-premises servers that belong to a physician or a particular medical facility.
- Remotely-hosted systems. All the data is stored and processed on remote third-party servers. Usually, it’s cloud servers, which allow for scalability, cost-efficiency, and security.
Benefits of EHR systems
An EHR system kills two birds with one stone as it helps both — medical facilities and their patients. Let’s take a look at the benefits of EHR systems for patients and healthcare providers.
Benefits of EHR systems for patients
Safer healthcare. The positive impact of the EHR on patient care is undeniable. A system that provides a single point of access to the entirety of patient data and their medical history dramatically improves the quality of the provided care. In fact, in the US, preventable medical errors are among the top causes of patient deaths. A well-functioning EHR decreases the chance of such mistakes significantly.
Easier access to healthcare. EHR gives you scheduling, online payments, messaging, telemedicine. Also, access to patient data makes medical care more accessible.
Reminders and notifications. EHR can remind patients about appointments, medication schedules, and important habits. Such functionality is especially valuable for patients who struggle with remembering things.
Benefits of EHR systems for healthcare providers
Reliable and secure system. EHR improves diagnostic accuracy and healthcare outcomes as well as streamlines operations. Besides, all data is stored on secure servers with backups and encryption. The chance of malicious data tampering or losing important data is close to zero.
Decreased costs and increased efficiency. It’s minimizing paperwork, decreasing the workload, streamlining operations. Also, it decreasing the chance of human error.
Space for strategic development. When you’re less worried about keeping everything together, you have more time to invest in the strategic planning and business development of your facility.
Increased reach. A solid patient functionality gives you access to new people that prefer the convenience and reliability of EHR systems.
What are the most critical stages in EHR development?
In 2021, the most critical stages in EHR development include:
1. Idea Validation and Discovery Phase
The ultimate EHR software system should have the majority of functionality we mentioned in the EHR software features chapter.
But, the development of such a comprehensive system takes a lot of time and investment. It shouldn’t limit the digitalization of the medical facility though. You can start with a solid minimum viable EHR. It will be a functioning product that generates value and improves operations.
Such an MVP EHR system should contain the basic core functions and some patient functionality, such as scheduling. The discovery phase should determine the project roadmap and the functionality to be developed first.
2. HIPAA/GDPR compliance assurance
Compliance with local regulations is crucial.
- If your EHR system is for the USA, it needs to comply with the HIPAA guidelines.
- If your EHR system is for the European market, it should comply with GDPR guidelines.
Both regulations specify the level of personal data security and confidentiality.
3. Adaptation for mobile devices
Patients are used to conducting business through mobile apps. Doctors and other medical professionals are likely to have phones on them at all times. A modern EHR system should provide a seamless mobile experience for maximum efficiency.
4. Through the QA phase
No amount of preparation and masterful execution can compensate for the lack of quality assurance. Only extensive testing can uncover all hidden weaknesses as well as new bugs. Complex systems are particularly dependent on thorough testing as they have a lot of moving parts.
Your EHR development partner
Analyzing the events of the past years, Deloitte rightfully asks, “Will healthcare systems accelerate digitalization, including community and hospital workflows, patient health records, telemedicine, decision support?”
We believe the answer is yes. The pandemic exacerbated the weaknesses of the industry and proved that proper preparation is crucial for maintaining stability and providing good care. A stable, secure EHR system is an important pillar of the required change.
If your healthcare facility lacks an EHR software system, and you need a reliable software development partner, we offer our expertise. If you’re interested in our experience, we have a track record that speaks for itself.


